Medical History:
A 62-year-old female patient with progressive vision loss in both eyes was examined in our clinic.
Diabetes mellitus (-)
Systemic hypertension (-)
Family history (-)
Smoking (-)
Trauma (-)
Examination Findings
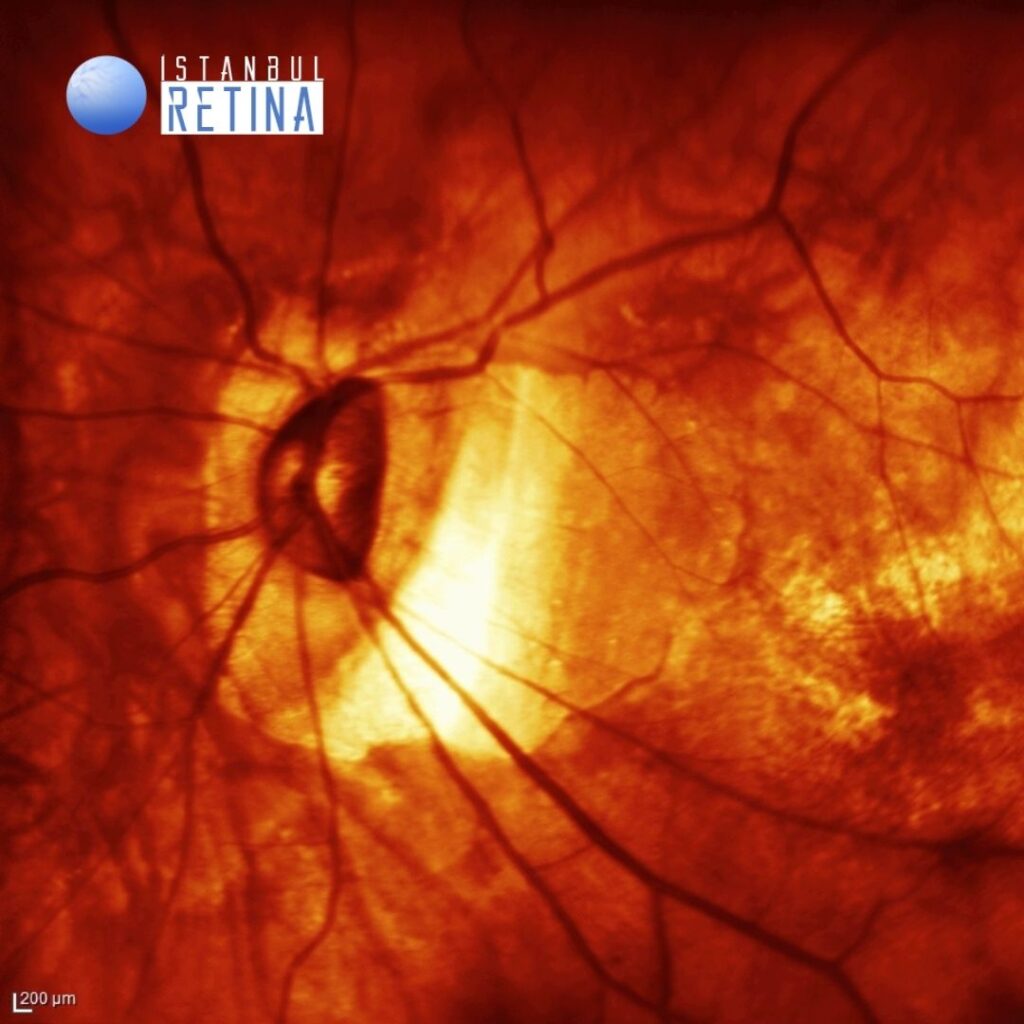
Best corrected visual acuity was 1/10 in both eyes. Intraocular pressure was 16 mmHg in both eyes. Anterior segment examination revealed bilateral PC-IOL. Funduscopic examination revealed myopic tilted disc, chorioretinal atrophy and posterior staphyloma in both eyes (Figure 1).
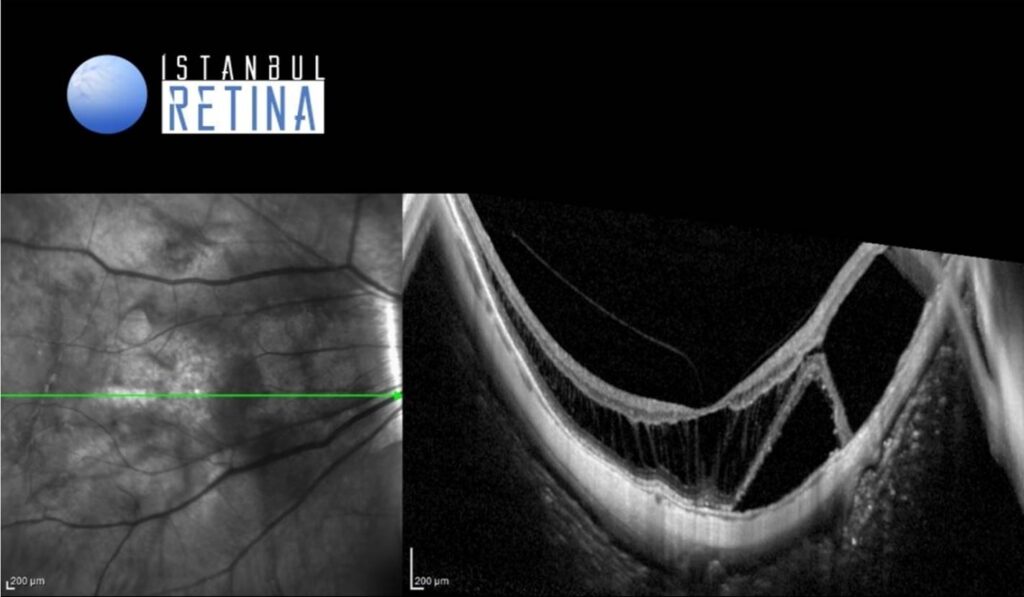
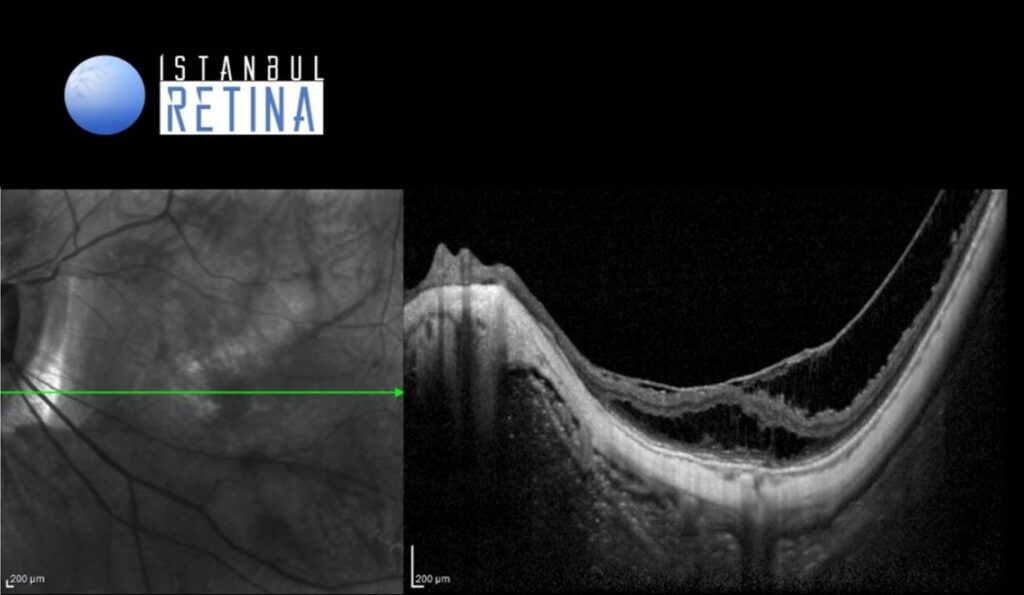
SD-OCT imaging shows marked myopic traction maculopathy in both eyes (Figure 2).
Diagnosis
Myopic Traction Maculopathy
Myopic traction maculopathy is a wide spectrum of clinical pictures that may affect up to 30% of eyes with pathologic myopia.
Recently, Parolini et al. have proposed a new classification that was specific for myopic traction maculopathy. It was defined as a progressive disease that first involves the innermost layers of the retina with an inner macular schisis and gradually progresses, involving the outermost retinal layers, until a macular detachment appears, whereas the schisis disappears.
At the stage of maculoschisis, myopic traction maculopathy can be classified in stage 1 (inner or inner-outer schisis) and stage 2 (purely outer schisis). Myopic traction maculopathy further progresses into macular detachment, or stage 3, which is a separation between the RPE and photoreceptors layers. Stage 3 evolves into stage 4, that describes a macular detachment extended to the whole posterior pole, whereas the schisis in the retina disappears, as the intraretinal stretching is released by the detachment of the outer retinal layers from the RPE.
Treatment
Management strategies for myopic traction maculopathy include: observation, macular buckle, pars plana vitrectomy or combination of both techniques based on the clinical features.
References:
Parolini B, Palmieri M, Finzi A, Besozzi G, Frisina R. Myopic Traction Maculopathy: A New Perspective on Classification and Management. Asia Pac J Ophthalmol (Phila). 2021;10(1):49-59. https://pubmed.ncbi.nlm.nih.gov/33481391/