Medical History:
Diabetes mellitus (-)
Systemic hypertension (-)
Family history (-)
Smoking (-)
Trauma (-)
Examination Findings
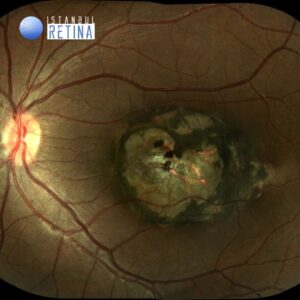
Best corrected visual acuity was 10/10 in the right eye and counting fingers at 1 meter in the left eye. Intraocular pressure was 13 mmHg in the right eye and 14 in the left eye. Anterior segment examination was unremarkable. Dilated funduscopic examination revealed normal fundus appearance in the right eye and darkly pigmented chorioretinal scar involving the macula in the left eye (Fig. 1).
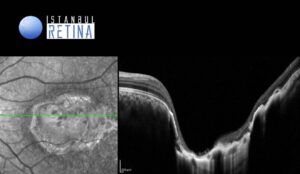
Optical coherence tomography (OCT) through the lesion demonstrated a large, excavated, coloboma-like chorioretinal lesion (Fig 2).
Diagnosis
Chorioretinal Scar of Congenital Ocular Toxoplasmosis
Toxoplasma gondii is an obligate intracellular parasite. Congenital toxoplasmosis is usually due to a primary maternal infection acquired during pregnancy. Congenital toxoplasmosis is most commonly acquired during the last trimester of pregnancy, with infants usually asymptomatic. Congenital infections are associated with intrauterine growth restriction, hepatosplenomegaly, central nervous system involvement and chorioretinitis. Fetuses affected early in gestation generally have more severe disease. The classic triad of findings consists of chorioretinitis, hydrocephalus, and intracranial calcifications. Serological testing, MRI or CT imaging of the brain, and a comprehensive eye exam should be performed for infants with suspected congenital toxoplasmosis.
Differential Diagnosis
Chorioretinal coloboma, persistent fetal vasculature, retinoblastoma
Treatment
Patients with inactive toxoplasmosis do not require treatment. Antimicrobial therapy is required for managing systemic toxoplasmosis in newborns, pregnant women and immunosuppressed patients and in acute symptomatic disease, especially when vision is threatened due to the anatomic location or severe inflammation.
References:
de Campos VS, Calaza KC, Adesse D. Implications of TORCH Diseases in Retinal Development-Special Focus on Congenital Toxoplasmosis. Front Cell Infect Microbiol. 2020;10:585727. https://pubmed.ncbi.nlm.nih.gov/33194824/


