Medical History:
A 50-year-old female patient presented with complaint of vision loss in the right eye.
Diabetes mellitus (-)
Systemic hypertension (-)
Family history (-)
Smoking (-)
Trauma (-)
Examination Findings
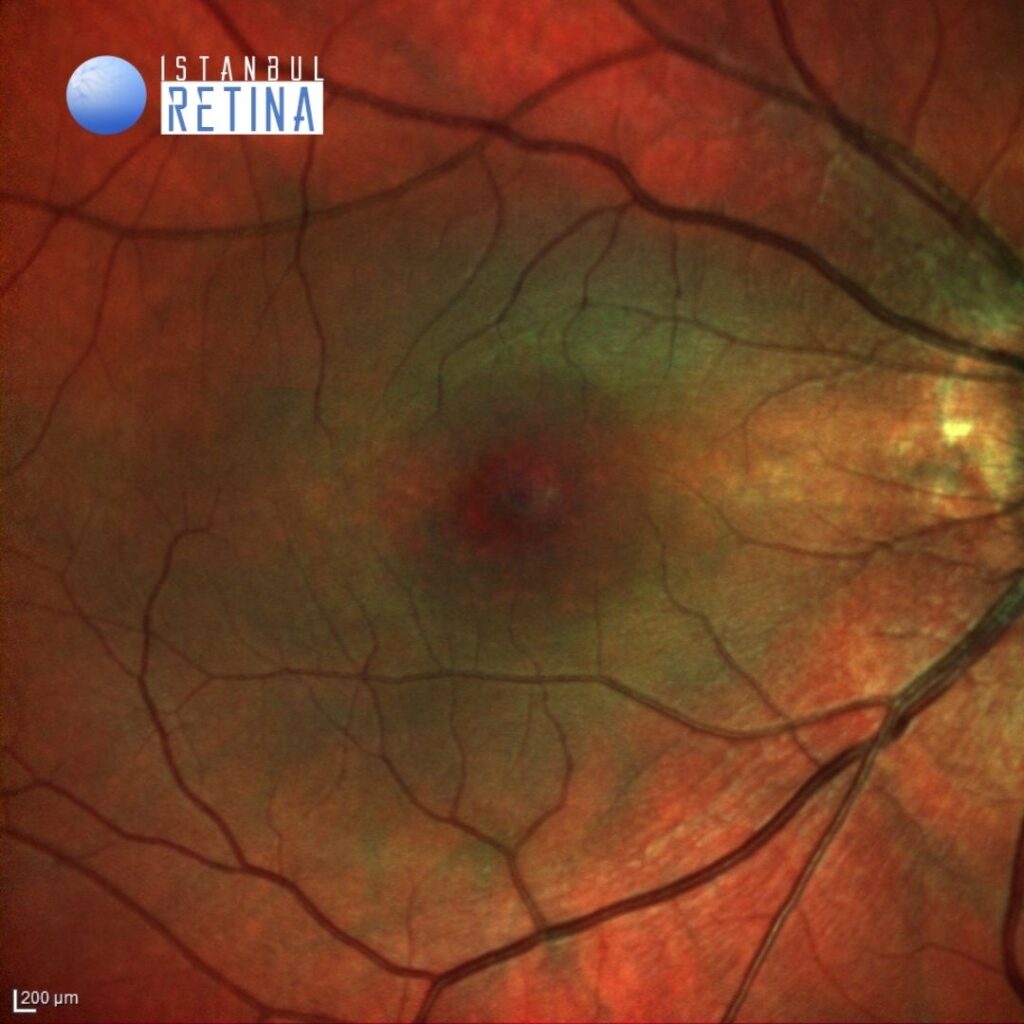
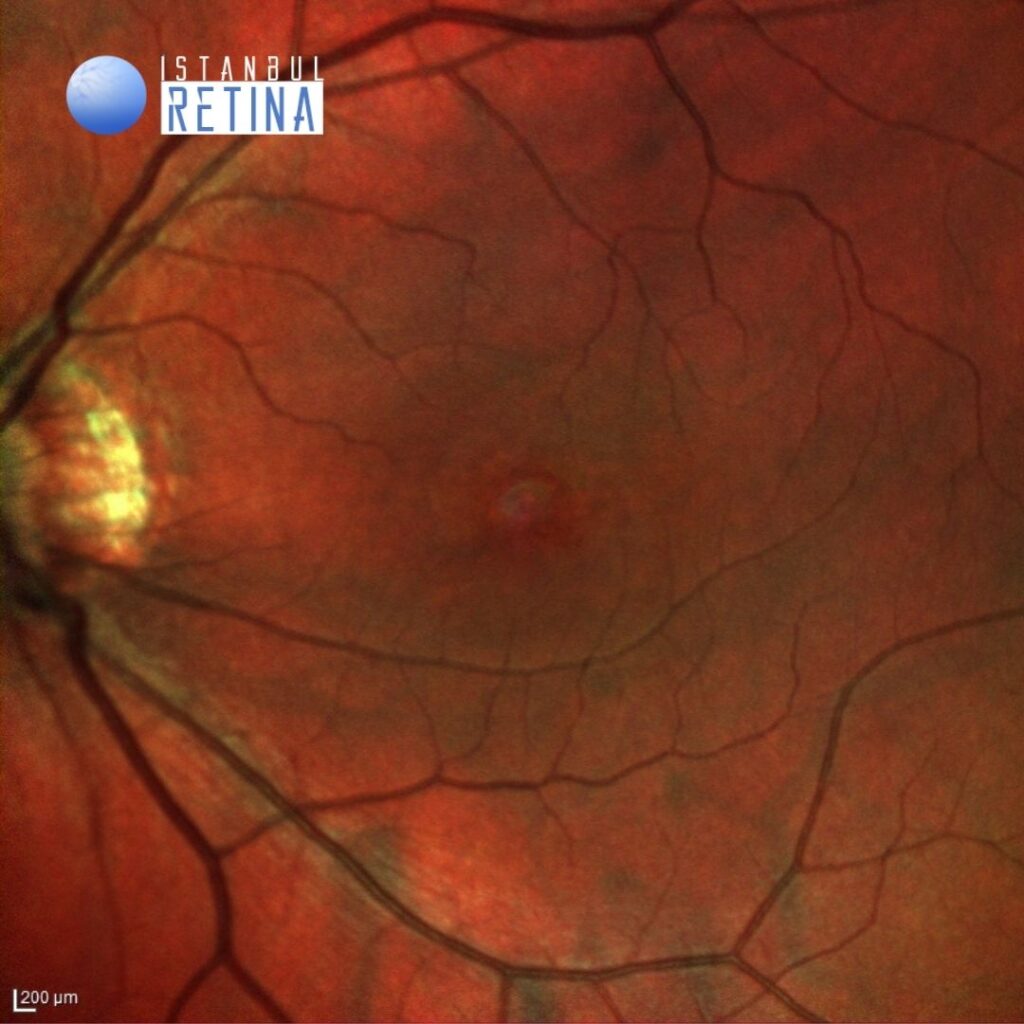
Best corrected visual acuity was 5/10 in the right eye and 10/10 in the left eye. Spherical equivalent was -7.25 D in the right eye and -6.75 D in the left eye. Intraocular pressure was 15 mmHg in the right eye and 16 in the lefte ye. Anterior segment examination was unremarkable. Fundus examination revealed bilateral posterior staphyloma (Figure 1).
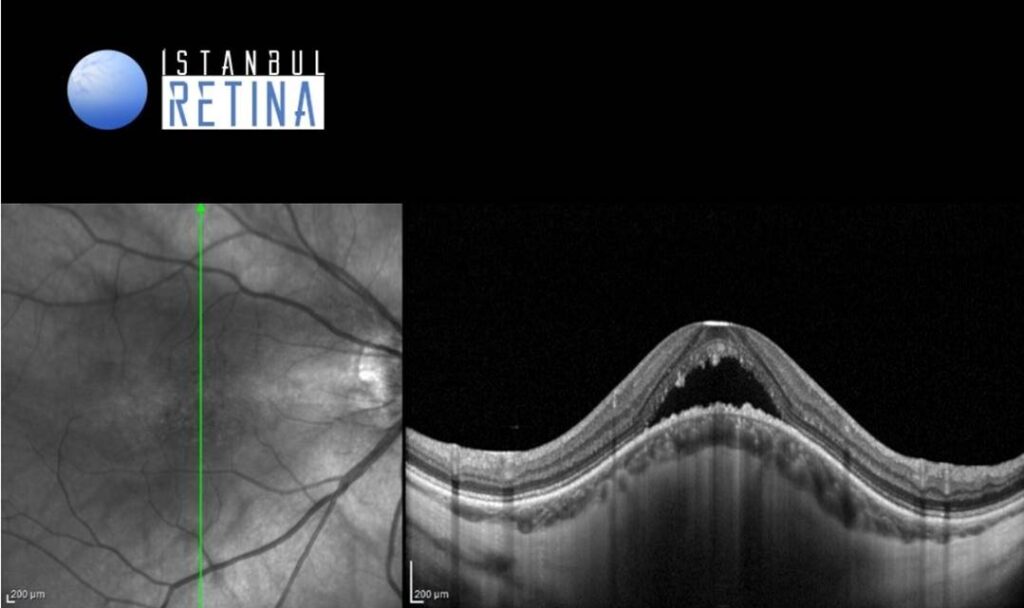
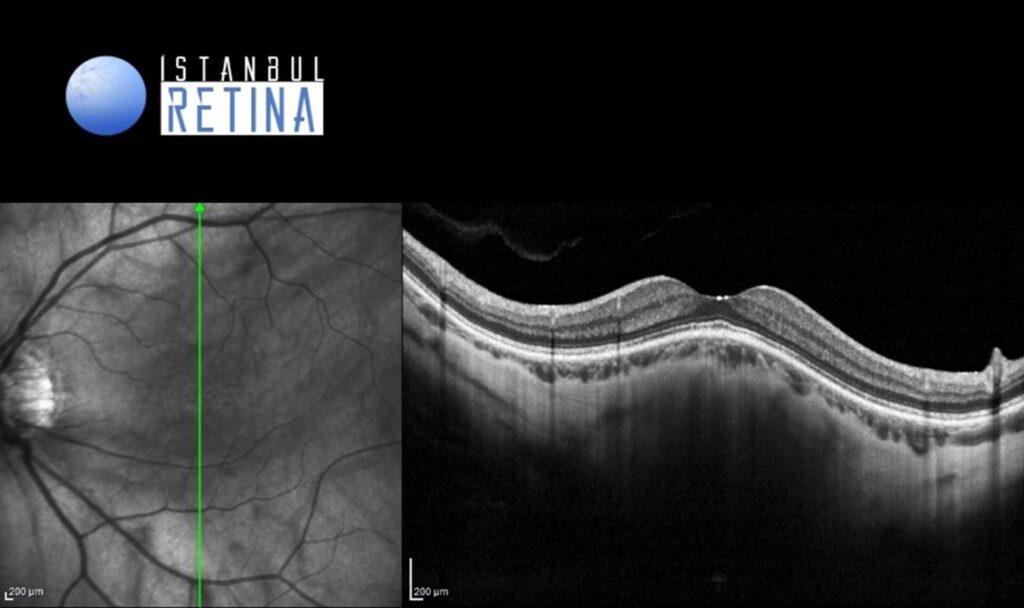
Optic coherence tomography (OCT) scan demonstrated dome-shaped macular configuration in both eyes and subretinal fluid in the right eye (Figure 2).
Diagnosis
Serous Retinal Detachment Associated with Dome-Shaped Macula
Dome-shaped macula is characterized by a convex anterior protrusion of the macula associated with high myopia and posterior staphyloma. Dome-shaped macula has been shown to occur in 10-20% of highly myopic eyes. Optical coherence tomography (OCT) is necessary to diagnose dome-shaped macula and identify the morphological type. Because the convexity can appear in different orientations, it is important to obtain both vertical and horizontal scans. The most frequent complication of dome-shaped macula is subfoveal serous retinal detachment. The prevalence of subfoveal serous retinal detachment in dome-shaped macula has been shown in 2% to 67% of patients with dome-shaped macula. The exact pathophysiology of subfoveal serous retinal detachment associated with dome-shaped macula remains unclear.
Differential Diagnosis
Central serous chorioretinopathy, choroidal hemangioma, choroidal melanoma, uveal effusion syndrome, posterior scleritis
Treatment
No effective treatment for serous retinal detachment associated with dome-shaped macula has been established.
References:
Hocaoglu M, Ersoz MG, Sayman Muslubas I, Arf S, Karacorlu M. Factors associated with macular complications in highly myopic eyes with dome-shaped macular configuration. Graefes Arch Clin Exp Ophthalmol. 2019;257:2357-2365. https://pubmed.ncbi.nlm.nih.gov/31485730/